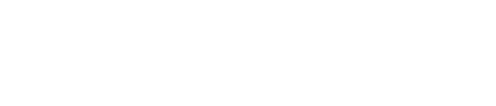Our technology is used by over 300 health and care organisations to engage, plan, and deploy their people: supporting resources in the fairest and most effective way.
Each product has been developed with the health and care workforce in mind and aims to make everyone’s working lives easier, so that your people receive the best experiences and can focus on what matters most, delivering quality care.
From job planning, rostering and temporary staffing to training, communication and HR management, our wide range of SaaS solutions are designed to help you manage your workforce, operate efficiently, and ensure everyone’s safety, so you can confidently meet the care needs of your patients and service users.